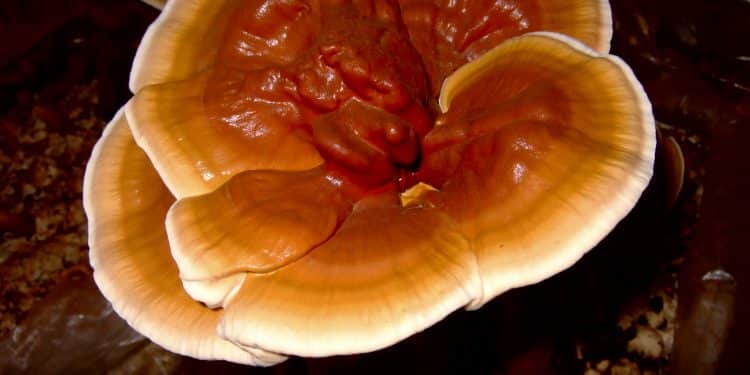
With increasing exposure to stress, chronic infections, increased gut permeability, and synthetic stressors, autoimmune conditions are becoming increasingly prevalent. Conventional approaches that suppress the immune system might not produce lasting changes, which patients are seeking.
So Is Reishi Mushroom Good for Autoimmune Conditions?
Reishi has been shown to balance and improve immune system function, but further studies need to be conducted to determine if reishi is good for auto-immune disorders. If reishi is something you’d like to try, you can always consult your doctor to determine if it may help you. Some studies and patients have reported benefits, but again, more studies need to be done to confirm any concrete findings, and results can vary depending on your specific autoimmune condition.
Examples of Reishi and other Mushrooms Benefiting Auto-Immune Disorders
Another animal study showed improvements in symptoms of Lupus as well as in immune markers following the administration of Reishi and certain herbs. In vitro studies have shown that a protein found in Reishi called Ling Zhi-8 (LZ-8) can exert positive autoimmunity suppression effects, decreasing the levels of TNF-alpha and disruptive antibodies. Mutations in the ergothioneine transporter system can build susceptibility to some auto-immune diseases, such as rheumatoid arthritis and Crohns disease.
Ergothioneine is a compound that is being studied for its antioxidant effects, since it is found in only a select few foods, and mushrooms are among the highest sources. Direct evidence of mushrooms and certain autoimmune conditions is needed for further data. Using fungi extracts for autoimmune conditions is sometimes a matter of a little patience, as well as knowing when, how much, how frequently, and what types of mushroom extracts will enhance the patients response. Naturopathic doctors need to take into account sources of immune-suppressing medications when looking for natural approaches.
Cyclosporine is actually derived from a fungus called cordyceps. Tolypocladium inflatum, the fungus that gives rise to Cyclosporine, is an asexual form of Cordyceps. Mycophenolates are produced by either Penicillium stoloniferum fungus or related Penicillium echinulatum fungus.
Although the next generation of transplant drugs are derived from bacteria and antibodies, mushrooms and fungi do possess immunomodulating properties, which may prove to be of importance in practice. Treatments using medicinal mushrooms could potentially reduce the need for pharmaceutical interventions.
Like cyclosporine, cordyceps is also capable of lowering the levels of IL-2.11 Even though it has had a long history of usage, studies are finding new applications of cordyceps. It shows potential for treating type I diabetes by slowing down cell-mediated destruction of insulin-producing beta cells. Cordyceps also works as a treatment for Lupus by decreasing titers of antibodies against double-stranded DNA. For patients taking cyclosporine, cordyceps may decrease toxicity from that drug if taken in combination.
Other mushrooms have shown promise in treating autoimmune conditions, although reishi and shiitake mushrooms are known to raise IL-2.11 Ganoderma lucidum has been shown in a murine model to decrease sialadenitis (salivary gland inflammation) by changing CD4(+)/CD8(+) ratio, T cells, and serum IgG levels. In one study in patients with glomerulonephritis, it was shown to restore the immune circulation balance and to interrupt ongoing proteinuria. Ganoderma tsugae was shown in mice to prevent the production of autoantibodies and to reduce the penetration of mononuclear cells in the parenchymal tissues.
In another animal model, Shiitake mushrooms showed potential for immuno-mediated colitis through alterations of the CD4/CD8 ratio. This is accomplished through increased CD8 entrapment of the liver, leading to a reduction of colitis symptoms.
Other mushrooms being investigated for use in autoimmune conditions are Phellinus linteus for rheumatoid arthritis, and Phellinus igniarius for autoimmune encephalopathy. Much of this activity is likely attributed to a copper-containing enzyme found in mushrooms called tyrosinase, or polyphenol oxidase. Results of the mouse study indicate that the extract alone could be useful for vitiligo.
Additional Studies:
https://pubmed.ncbi.nlm.nih.gov/11480842/
https://pubmed.ncbi.nlm.nih.gov/15567896/
Is Reishi Mushroom AIP?
While medicinal mushrooms (such as shiitake, which is widely accessible in supermarkets) are acceptable under the Autoimmune Protocol, there is still more reseaerch that needs to be done to validate this before reishi and other medicinal mushroom extracts are authorized for autoimmune disease treatment. For now, medicinal mushroom extracts should be considered an AIP gray area.
You could always try to incorporate reishi into your diet, and with the help of your doctor, determine whether the symptoms of your autoimmune disease improve or worsen.
Reishi mushrooms, have been shown to be more immunomodulatory (than immunostimulatory) in newer research. Reishi is the most thoroughly researched among them.
In rheumatoid arthritis patients, two studies found a reduction in joint pain alongside a drop in interleukin (IL)-18, which strongly activates Th1 cells. There was also no change in any measured inflammatory cells or other cytokines.) In a study of mice with lupus, reishi extract supplementation reduced autoantibodies and improved survival. Reishi increased the ratio of regulatory T cells to Th17 and Th1 cells, as well as cytokines, such as decreases in IL-21, IL-10, and IL-17 and increases in IL-2 and IL-12P70, according to a mouse lupus research. Finally, reishi supplementation was found to reverse changes in gene expression that corresponded with reduced disease activity in a mouse model of autoimmune Alzheimer’s disease. The fascinating context is that reishi extract has also been shown to be effective in cancer, specifically boosting cytotoxic T cell activity (in addition to affecting tumor angiogenesis and cancer cell growth directly).
The data presented in this image suggest that medicinal mushroom extracts (at least in the case of reishi) may help with cases of under-active immune systems, overactive immune function, and carcinogenesis.
Additionally, reishi mushrooms contain a compound called purine. Purines are a type of molecule that can be broken down into uric acid. Uric acid is known to aggravate gout symptoms.
For this reason, people with gout may want to avoid eating reishi mushrooms. If you are unsure whether or not you should eat reishi mushrooms, you should speak with your doctor or a registered dietitian.
A Discussion on Functional Mushrooms and Autoimmune Disease
Functional mushrooms are typically used to support the individual immune system, generally understood to act as immune regulators. Some of the more common autoimmune conditions seen by healthcare practitioners include Hashimotos thyroiditis, Sjogrens Syndrome, Rheumatoid Arthritis (RA), Celiac disease, Pernicious Anemia, and certain irritable bowel conditions. There appear to be two trains of thought in discussing the applications of functional mushrooms to autoimmune conditions. For those who are worried about using functional mushrooms in autoimmune conditions, negative reactions, irritation, and relapse are usually reasons for backing off of regular use of functional mushrooms.
Without further investigation, it is common for practitioners to completely eliminate reishi mushrooms from their treatment plans and attempt other strategies. After doctors with an emphasis on autoimmunity, chronic infections, and integrative cancer care, it is clear the approaches outlined above could use some further elaboration. The doctors suggested chronic infections, immune suppression, toxicity, and microbiome imbalances might require additional attention prior to trying to incorporate reishi mushrooms. The doctors further clarified that using the wide range of the fungus blend products is something to be considered when using mushrooms for patients suffering from autoimmune diseases.
Dosage, frequency, and type of extract are also things to consider when working with autoimmune patients, often depending on a case-by-case basis. When resolution or amelioration occurs in relation to the underlying intervening factors, pharmacological mushrooms can produce fewer flare-ups in the autoimmune patient. Because the immune system is so complicated, it is difficult even with a surge of research on mycology to tell whether Mushroom A would work better in Condition B. However, there is a bit of immunology out there that can help drive that conversation.
You can find our favorite capsules, powders, and tincture’s on the following pages of our website and learn more about each individually:
Best Reishi Mushroom Supplement
Best Reishi Mushroom Mushroom Gummies
Additional Resources:
Are Reishi Mushrooms Hallucinogenic?
Updated 10/19/2022